Editorial
Dear Reader, dear friends,
this has been yet another successful year for OptiMedis. We held the 10-year celebration of our flagship integrated health care model ´Healthy Kinzigtal´; we opened our first health academy (a four story building) which runs courses and events for policyholders, education and training for professionals, and offers exercise and therapy in our state-of-the-art movement centre. Our flagship project continues to improve population health and health care experience (both assessed by independent research institutes) while decreasing overall costs (on average, annual savings for each insured amount to 170 Euro compared to the national average). We have made good progress to start setting up three other population-based health care systems in the south of Germany and another one in an urban area in the North. Moreover, in addition to the activities of our branch in the Netherlands, we are engaged in discussions with foundations, research institutes, health care companies in Europe and beyond to support similar projects.
The question is: can the Healthy Kinzigtal approach be successfully transferred and achieved elsewhere, including in regions that are different in population structure and health service organization? While all regions will have their idiosyncratic features and particularities, we argue that the general model, interventions and evaluation frameworks are widely applicable. All k 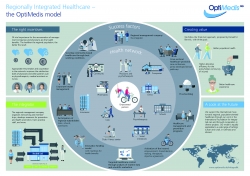 ey aspects of the model are deeply rooted in the scientific literature and in models that have proven effective elsewhere, such as the Triple Aim approach, the chronic care model, audit and feedback strategies, the focus on patient activation, interventions to reduce unnecessary hospital admissions and readmissions, or pharmacological consultations to improve the safety of drug prescriptions. It is because of the innovative nature, the strong reference to theoretical models and principles of evidence-based medicine and its rigorous evaluation that we deem our model a useful reference for other countries to adapt and scale up.
ey aspects of the model are deeply rooted in the scientific literature and in models that have proven effective elsewhere, such as the Triple Aim approach, the chronic care model, audit and feedback strategies, the focus on patient activation, interventions to reduce unnecessary hospital admissions and readmissions, or pharmacological consultations to improve the safety of drug prescriptions. It is because of the innovative nature, the strong reference to theoretical models and principles of evidence-based medicine and its rigorous evaluation that we deem our model a useful reference for other countries to adapt and scale up.
The developments this year have inspired us to capture our model of Regionally Integrated Healthcare in an infographic (see picture), to make it more tangible for you. We’d love your feedback.
We wish you all a Merry Christmas and a Happy New Year 2016!
Sincerely yours,
 |
Dr Oliver Groene, |
|
The infographic on our web – please click here
If you like to receive this newsletter on a regular basis, please click here www.optimedis.com/newsletter.
Contents
About OptiMedis and our projects |
||||
| 10 Years of Gesundes Kinzigtal: Integrated Healthcare celebrates its anniversary | > more | |||
| Gesundes Kinzigtal improves contribution margin | > more | |||
| The Advisory Board: Q&A about Gesundes Kinzigtal | > more | |||
| Hamburg Federal Healthcare Conference supports OptiMedis Project | > more | |||
General topics |
||||
| The rapid proliferation of Accountable Care Organizations in the US: What’s the secret sauce? | > more | |||
Reading Tips |
||||
| The Health Foundation: Three new resources to enable person-centred care | > more | |||
Events, you can meet us |
||||